Business Name: BeeHive Homes of Gallup
Address: 600 Gurley Ave, Gallup, NM 87301
Phone: (505) 591-7024
BeeHive Homes of Gallup
Beehive Homes of Gallup assisted living care is ideal for those who value their independence but require help with some of the activities of daily living. Residents enjoy 24-hour support, private bedrooms with baths, medication monitoring, home-cooked meals, housekeeping and laundry services, social activities and outings, and daily physical and mental exercise opportunities. Beehive Homes memory care services accommodates the growing number of seniors affected by memory loss and dementia. Beehive Homes offers respite (short-term) care for your loved one should the need arise. Whether help is needed after a surgery or illness, for vacation coverage, or just a break from the routine, respite care provides you peace of mind for any length of stay.
600 Gurley Ave, Gallup, NM 87301
Business Hours
Monday thru Sunday: 9:00am to 5:00pm
TikTok: https://www.tiktok.com/@beehivehomesgallup
YouTube: https://www.youtube.com/@WelcomeHomeBeeHiveHomes
Facebook: https://www.facebook.com/beehivehomesgallup
Instagram: https://www.instagram.com/beehivehomesofgallup/
Care for older grownups is a craft found out in time and tempered by humbleness. The work covers medication reconciliations and late-night peace of mind, get bars and difficult conversations about driving. It requires stamina and the determination to see a whole individual, not a list of diagnoses. When I think of what makes senior care reliable and humane, 3 worths keep surfacing: safety, dignity, and empathy. They sound easy, however they show up in complex, sometimes inconsistent ways across assisted living, memory care, respite care, and home-based support.
I have sat with families working out the cost of a center while debating whether Mom will accept aid with bathing. I have actually seen a happy retired instructor accept utilize a walker only after we discovered one in her favorite color. These details matter. They end up being the texture of daily life in senior living neighborhoods and in the house. If we handle them with skill and regard, older grownups thrive longer and feel seen. If we stumble, even with the best intents, trust erodes quickly.
What safety in fact looks like
Safety in elderly care is less about bubble wrap and more about avoiding predictable damages without stealing autonomy. Falls are the heading threat, and for excellent factor. Approximately one in 4 grownups over 65 falls each year, and a meaningful fraction of those falls results in injury. Yet fall prevention done inadequately can backfire. A resident who is never enabled to walk separately will lose strength, then fall anyhow the very first time she should hurry to the restroom. The safest strategy is the one that preserves strength while lowering hazards.
In useful terms, I begin with the environment. Lighting that pools on the floor instead of casting glare, limits leveled or marked with contrasting tape, furnishings that will not tip when utilized as a handhold, and bathrooms with sturdy grab bars positioned where individuals really reach. A textured shower bench beats a fancy day spa fixture each time. Shoes matters more than many people think. I have a soft area for well-fitting shoes with heel counters and rubber soles, and I will trade a trendy slipper for a dull-looking shoe that grips damp tile without apology.
Medication security is worthy of the exact same attention to information. Numerous senior citizens take 8 to twelve prescriptions, frequently prescribed by different clinicians. A quarterly medication reconciliation with a pharmacist cuts errors and side effects. That is when you capture replicate blood pressure tablets or a medication that gets worse dizziness. In assisted living settings, I encourage "do not crush" lists on med carts and a culture where personnel feel safe to double-check orders when something looks off. In your home, blister packs or automated dispensers reduce guesswork. It is not only about avoiding mistakes, it has to do with preventing the snowball effect that begins with a single missed pill and ends with a medical facility visit.
Wandering in memory care calls for a well balanced technique also. A locked door fixes one issue and produces another if it sacrifices dignity or access to sunshine and fresh air. I have seen secured courtyards turn anxious pacing into peaceful laps around raised garden beds. Doors camouflaged as bookshelves minimize exit-seeking without heavy-handed barriers. Innovation assists when utilized attentively: passive motion sensing units set off soft lighting on a path to the bathroom at night, or a wearable alert informs personnel if somebody has not moved for an uncommon interval. Safety must be undetectable, or a minimum of feel helpful instead of punitive.
Finally, infection prevention sits in the background, ending up being noticeable only when it stops working. Simple routines work: hand health before meals, sanitizing high-touch surface areas, and a clear plan for visitors throughout influenza season. In a memory care unit I worked with, we swapped cloth napkins for single-use throughout norovirus break outs, and we kept hydration stations at eye level so people were cued to consume. Those small tweaks shortened outbreaks and kept residents much healthier without turning the place into a clinic.
Dignity as day-to-day practice
Dignity is not a slogan on the pamphlet. It is the practice of maintaining an individual's sense of self in every interaction, especially when they need help with intimate jobs. For a happy Marine who dislikes asking for support, the distinction between an excellent day and a bad one might be the way a caregiver frames help: "Let me constant the towel while you do your back," rather than "I'm going to clean you now." Language either teams up or takes over.
Appearance plays a quiet function in dignity. Individuals feel more like themselves when their clothes matches their identity. A former executive who always used crisp t-shirts might thrive when personnel keep a rotation of pressed button-downs prepared, even if adaptive fasteners change buttons behind the scenes. In memory care, familiar textures and colors matter. When we let residents choose from two preferred outfits instead of laying out a single option, approval of care improves and agitation decreases.
Privacy is a simple idea and a tough practice. Doors must close. Staff needs to knock and wait. Bathing and toileting are worthy of a calm speed and explanations, even for homeowners with innovative dementia who might not understand every word. They still comprehend tone. In assisted living, roomies can share a wall, not their lives. Earphones and space dividers cost less than a healthcare facility tray table and confer exponentially more respect.
Dignity also appears in scheduling. Stiff regimens might assist staffing, however they flatten specific choice. Mrs. R sleeps late and consumes at 10 a.m. Great, her care plan must show that. If breakfast technically runs till 9:30, extend it for her. In home-based elderly care, the choice to shower at night or morning can be the distinction in between cooperation and battles. Little versatilities recover personhood in a system that often pushes towards uniformity.
Families often stress that accepting aid will erode self-reliance. My experience is the opposite, if we set it up correctly. A resident who uses a shower chair securely using very little standby assistance stays independent longer than one who withstands help and slips. Self-respect is protected by suitable assistance, not by stubbornness framed as independence. The trick is to include the individual in choices, show respect for their goals, and keep tasks scarce enough that they can succeed.
Compassion that does, not just feels
Compassion is compassion with sleeves rolled up. It shows in how a caretaker reacts when a resident repeats the very same concern every five minutes. A quick, patient response works better than a correction. In memory care, reality orientation loses to recognition most days. If Mr. K is looking for his late wife, I have actually stated, "Inform me about her. What did she produce supper on Sundays?" The story is the point. After ten minutes of sharing, he typically forgets the distress that launched the search.
There is likewise a thoughtful method to set limits. Personnel burn out when they puzzle limitless giving with professional care. Borders, training, and team effort keep empathy reputable. In respite care, the goal is twofold: offer the household real rest, and provide the elder a predictable, warm environment. That suggests constant faces, clear regimens, and activities developed for success. A good respite program discovers a person's preferred tea, the kind of music that stimulates rather than upsets, and how to relieve without infantilizing.
I learned a lot from a resident who hated group activities but liked birds. We positioned a small feeder outside his window and added a weekly bird-watching circle that lasted twenty minutes, no longer. He participated in whenever and later on tolerated other activities due to the fact that his interests were honored first. Empathy is personal, particular, and often quiet.
Assisted living: where structure fulfills individuality
Assisted living sits in between independent living and nursing care. It is developed for adults who can live semi-independently, with support for day-to-day jobs like bathing, dressing, meals, and medication management. The best communities seem like apartment buildings with a helpful neighbor around the corner. The worst seem like health centers attempting to pretend they are not.

During trips, households focus on decoration and activity calendars. They ought to likewise inquire about staffing ratios at various times of day, how they manage falls at 3 a.m., and who creates and updates care strategies. I try to find a culture where the nurse understands homeowners by nickname and the front desk acknowledges the son who goes to on Tuesdays. Turnover rates matter. A building with continuous personnel churn struggles to preserve constant care, no matter how beautiful the dining room.
Nutrition is another litmus test. Are meals prepared in a manner that preserves cravings and dignity? Finger foods can be a wise option for people who have problem with utensils, but they ought to be used with care, not as a downgrade. Hydration rounds in the afternoon, flavored water options, and treats rich in protein aid keep weight and strength. A resident who loses five pounds in a month deserves attention, not a new dessert menu. Check whether the community tracks such modifications and calls the family.
Safety in assisted living ought to be woven in without dominating the atmosphere. That means pull cables in bathrooms, yes, but also personnel who notice when a mobility pattern changes. It means exercise classes that challenge balance safely, not simply chair aerobics. It means maintenance teams that can set up a 2nd grab bar within days, not months. The line between independent living and assisted living blurs in practice, and a flexible community will adjust support up or down as requires change.
Memory care: creating for the brain you have
Memory care is both a space and an approach. The space is protected and streamlined, with clear visual cues and lowered mess. The viewpoint accepts that the brain processes information in a different way in dementia, so the environment and interactions must adjust. I have enjoyed a corridor mural showing a country lane lower agitation more effectively than a scolding ever could. Why? It invites wandering into a consisted of, calming path.
Lighting is non-negotiable. Bright, consistent, indirect light minimizes shadows that can be misinterpreted as challenges or strangers. High-contrast plates aid with eating. Labels with both words and photos on drawers allow an individual to find socks without asking. Fragrance can cue appetite or calm, but keep it subtle. Overstimulation is a common mistake in memory care. A single, familiar melody or a box of tactile items connected to a person's previous hobbies works much better than consistent background TV.
Staff training is the engine. Techniques like "hand under hand" for assisting movement, segmenting tasks into two-step triggers, and avoiding open-ended questions can turn a stuffed bath into a successful one. Language that starts with "Let's" instead of "You require to" assisted living decreases resistance. When locals decline care, I assume worry or confusion rather than defiance and pivot. Perhaps the bath becomes a warm washcloth and a lotion massage today. Security remains intact while self-respect stays undamaged, too.
Family engagement is challenging in memory care. Loved ones grieve losses while still showing up, and they bring important history that can transform care plans. A life story document, even one page long, can rescue a difficult day: chosen nicknames, favorite foods, professions, pets, regimens. A previous baker may relax if you hand her a blending bowl and a spoon throughout an agitated afternoon. These information are not fluff. They are the interventions.
Respite care: oxygen masks for families
Respite care uses short-term support, usually measured in days or weeks, to give family caretakers space to rest, travel, or deal with crises. It is the most underused tool in elderly care. Families often wait till exhaustion forces a break, then feel guilty when they lastly take one. I try to stabilize respite early. It sustains care at home longer and secures relationships.
Quality respite programs mirror the rhythms of permanent locals. The room must feel lived-in, not like a spare bed by the nurse's station. Consumption must gather the same personal information as long-lasting admissions, including routines, activates, and preferred activities. Good programs send out a short daily update to the household, not due to the fact that they must, however because it reduces stress and anxiety and prevents "respite remorse." A picture of Mom at the piano, nevertheless easy, can alter a household's entire experience.
At home, respite can arrive through adult day services, at home assistants, or over night companions. The secret is consistency. A turning cast of strangers undermines trust. Even 4 hours twice a week with the same person can reset a caregiver's tension levels and enhance care quality. Funding varies. Some long-term care insurance prepares cover respite, and particular state programs offer vouchers. Ask early, since waiting lists are common.
The economics and principles of choice
Money shadows almost every choice in senior care. Assisted living expenses frequently vary from modest to eye-watering, depending on location and level of support. Memory care units generally add a premium. Home care uses versatility but can become expensive when hours intensify. There is no single right response. The ethical challenge is lining up resources with objectives while acknowledging limits.

I counsel families to construct a sensible budget plan and to review it quarterly. Requirements alter. If a fall reduces mobility, costs may spike momentarily, then support. If memory care becomes needed, selling a home may make sense, and timing matters to capture market price. Be honest with facilities about budget constraints. Some will deal with step-wise assistance, pausing non-essential services to consist of costs without threatening safety.
Medicaid and veterans benefits can bridge spaces for qualified individuals, but the application procedure can be labyrinthine. A social worker or elder law attorney frequently spends for themselves by avoiding expensive mistakes. Power of lawyer files must be in location before they are required. I have actually seen families invest months trying to assist a loved one, only to be obstructed due to the fact that paperwork lagged. It is not romantic, but it is profoundly caring to handle these legalities early.
Measuring what matters
Metrics in elderly care typically focus on the quantifiable: falls per month, weight modifications, medical facility readmissions. Those matter, and we should watch them. But the lived experience shows up in smaller signals. Does the resident go to activities, or have they retreated? Are meals largely consumed? Are showers endured without distress? Are nurse calls ending up being more frequent at night? Patterns tell stories.
I like to include one qualitative check: a regular monthly five-minute huddle where staff share something that made a resident smile and one challenge they came across. That easy practice constructs a culture of observation and care. Families can adopt a similar practice. Keep a short journal of gos to. If you discover a gradual shift in gait, state of mind, or hunger, bring it to the care group. Small interventions early beat dramatic actions later.
Working with the care team
No matter the setting, strong relationships in between families and staff enhance outcomes. Assume excellent intent and specify in your demands. "Mom seems withdrawn after lunch. Could we try seating her near the window and including a protein treat at 2 p.m.?" offers the group something to do. Deal context for behaviors. If Dad gets irritable at 5 p.m., that may be sundowning, and a short walk or quiet music might help.
Staff appreciate appreciation. A handwritten note calling a particular action brings weight. It likewise makes it simpler to raise concerns later. Set up care plan conferences, and bring reasonable goals. "Walk to the dining room independently 3 times this week" is concrete and attainable. If a facility can not fulfill a specific need, ask what they can do, not simply what they cannot.
Trade-offs and edge cases
Care plans deal with compromises. A resident with advanced cardiac arrest may want salted foods that comfort him, even as salt intensifies fluid retention. Blanket bans typically backfire. I choose worked out compromises: smaller sized portions of favorites, paired with fluid tracking and weight checks. With memory care, GPS-enabled wearables respect security while keeping the liberty to walk. Still, some elders refuse gadgets. Then we deal with environmental strategies, personnel cueing, and neighborly watchfulness.
Sexuality and intimacy in senior living raise genuine tensions. Two consenting adults with mild cognitive problems might seek companionship. Policies require nuance. Capability assessments need to be embellished, not blanket restrictions based upon diagnosis alone. Personal privacy must be safeguarded while vulnerabilities are kept track of. Pretending these needs do not exist undermines self-respect and strains trust.
Another edge case is alcohol use. A nighttime glass of wine for someone on sedating medications can be dangerous. Outright prohibition can sustain dispute and secret drinking. A middle path might include alcohol-free alternatives that simulate routine, in addition to clear education about dangers. If a resident selects to consume, documenting the decision and monitoring carefully are much better than policing in the shadows.
Building a home, not a holding pattern
Whether in assisted living, memory care, or at home with routine respite care, the goal is to develop a home, not a holding pattern. Residences contain regimens, peculiarities, and convenience items. They also adapt as requirements alter. Bring the pictures, the low-cost alarm clock with the loud tick, the worn quilt. Ask the hairdresser to visit the center, or set up a corner for hobbies. One male I understood had fished all his life. We developed a small take on station with hooks removed and lines cut short for safety. He tied knots for hours, calmer and prouder than he had actually remained in months.
Social connection underpins health. Motivate check outs, however set visitors up for success with brief, structured time and cues about what the elder enjoys. Ten minutes checking out favorite poems beats an hour of strained discussion. Pets can be effective. A calm feline or a checking out treatment dog will stimulate stories and smiles that no therapy worksheet can match.
Technology has a role when chosen carefully. Video calls bridge ranges, but just if someone aids with the setup and remains close during the discussion. Motion-sensing lights, wise speakers for music, and tablet dispensers that sound friendly instead of scolding can help. Prevent tech that adds anxiety or seems like security. The test is basic: does it make life feel safer and richer without making the person feel enjoyed or managed?
A practical starting point for families
- Clarify objectives and limits: What matters most to your loved one? Security at all costs, or self-reliance with specified risks? Compose it down and share it with the care team. Assemble files: Healthcare proxy, power of attorney, medication list, allergies, emergency contacts. Keep copies in a folder and on your phone. Build the lineup: Main clinician, pharmacist, facility nurse, 2 reputable household contacts, and one backup caregiver for respite. Names and direct lines, not just main numbers. Personalize the environment: Pictures, familiar blankets, identified drawers, favorite treats, and music playlists. Little, specific conveniences go further than redecorating. Schedule respite early: Put it on the calendar before exhaustion sets in. Treat it as maintenance, not failure.
The heart of the work
Safety, self-respect, and empathy are not separate projects. They strengthen each other when practiced well. A safe environment supports self-respect by permitting somebody to move freely without worry. Dignity invites cooperation, that makes safety procedures simpler to follow. Empathy oils the equipments when plans fulfill the messiness of real life.
The best days in senior care are typically ordinary. A morning where medications decrease without a cough, where the shower feels warm and unhurried, where coffee is served simply the way she likes it. A boy check outs, his mother recognizes his laugh even if she can not discover his name, and they keep an eye out the window at the sky for a long, quiet minute. These minutes are not additional. They are the point.
If you are picking between assisted living or more specialized memory care, or juggling home routines with intermittent respite care, take heart. The work is hard, and you do not have to do it alone. Construct your team, practice small, respectful practices, and change as you go. Senior living done well is simply living, with assistances that fade into the background while the person remains in focus. That is what safety, self-respect, and compassion make possible.
BeeHive Homes of Gallup provides assisted living care
BeeHive Homes of Gallup provides memory care services
BeeHive Homes of Gallup provides respite care services
BeeHive Homes of Gallup supports assistance with bathing and grooming
BeeHive Homes of Gallup offers private bedrooms with private bathrooms
BeeHive Homes of Gallup provides medication monitoring and documentation
BeeHive Homes of Gallup serves dietitian-approved meals
BeeHive Homes of Gallup provides housekeeping services
BeeHive Homes of Gallup provides laundry services
BeeHive Homes of Gallup offers community dining and social engagement activities
BeeHive Homes of Gallup features life enrichment activities
BeeHive Homes of Gallup supports personal care assistance during meals and daily routines
BeeHive Homes of Gallup promotes frequent physical and mental exercise opportunities
BeeHive Homes of Gallup provides a home-like residential environment
BeeHive Homes of Gallup creates customized care plans as residents’ needs change
BeeHive Homes of Gallup assesses individual resident care needs
BeeHive Homes of Gallup accepts private pay and long-term care insurance
BeeHive Homes of Gallup assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Gallup encourages meaningful resident-to-staff relationships
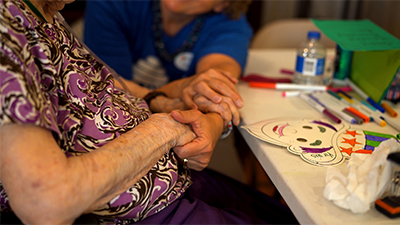
BeeHive Homes of Gallup delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Gallup has a phone number of (505) 591-7024
BeeHive Homes of Gallup has an address of 600 Gurley Ave, Gallup, NM 87301
BeeHive Homes of Gallup has a website https://beehivehomes.com/locations/gallup/
BeeHive Homes of Gallup has Google Maps listing https://maps.app.goo.gl/iMEbZo7VyH1tHATP9
BeeHive Homes of Gallup has TikTok page https://www.tiktok.com/@beehivehomesgallup
BeeHive Homes of Gallup has an YouTube page https://www.youtube.com/@WelcomeHomeBeeHiveHomes
BeeHive Homes of Gallup has Facebook page https://www.facebook.com/beehivehomesgallup
BeeHive Homes of Gallup has Instagram page https://www.instagram.com/beehivehomesofgallup/
BeeHive Homes of Gallup won Top Assisted Living Homes 2025
BeeHive Homes of Gallup earned Best Customer Service Award 2024
BeeHive Homes of Gallup placed 1st for Senior Living Communities 2025
People Also Ask about BeeHive Homes of Gallup
What is BeeHive Homes of Gallup Living monthly room rate?
The rate depends on the level of care that is needed. We do a pre-admission evaluation for each resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes of Gallup until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Do we have a nurse on staff?
No, but each BeeHive Home has a consulting Nurse available 24 – 7. if nursing services are needed, a doctor can order home health to come into the home
What are BeeHive Homes of Gallup's visiting hours?
Our visiting hours are currently under restriction by the state health officials. Limited visitation is still allowed but must be scheduled during regular business hours. Please contact us for additional and up-to-date information about visitation
Do we have couple’s rooms available?
Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Gallup located?
BeeHive Homes of Gallup is conveniently located at 600 Gurley Ave, Gallup, NM 87301. You can easily find directions on Google Maps or call at (505) 591-7024 Monday through Sunday 9:00am to 5:00pm
How can I contact BeeHive Homes of Gallup?
You can contact BeeHive Homes of Gallup by phone at: (505) 591-7024, visit their website at https://beehivehomes.com/locations/gallup/ or connect on social media via TikTok Facebook or YouTube
Visiting the Gallup City Park offers shaded seating and open green space where residents in assisted living, memory care, senior care, elderly care, and respite care can enjoy gentle outdoor relaxation.